
In this monthly report, FPM looks in detail at what the CQC have publicly reported from their GP practice inspections during March 2026, all anonymised. We highlight some of the behaviours that won practices Outstanding ratings, and the reasons some practices were scored Requires Improvement, or Inadequate. Do you recognise any of the observations the CQC picked up, either good or bad?
SOME 'OUTSTANDING' COMMENTS AND PRAISE FROM THE CQC:
Effective:
-
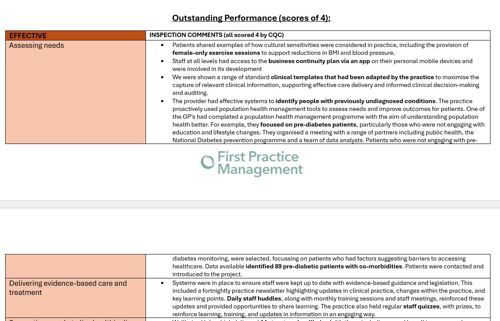
Assessing needs: the CQC praised one practice for their range of standard clinical templates that had been adapted by the practice to maximise the capture of relevant clinical information.
-
Supporting people to live healthier lives: one practice had a Wellbeing Hub which delivered structured wellbeing initiatives including a walking group and cooking group, with reductions in multiple clinical measures across the group and 300+ referrals from other PCN practices
Responsive:
-
Equity in access: 75% of respondents at one practice found it easy to contact the practice using the practice website. This was significantly higher when compared to both the much lower local average (51%) and national average (51%). Following a significant rise in telephone demand after COVID, one practice redesigned their call flows and reshaped the reception manager role to focus on actively managing call flow. This approach was shared through EQUIP to support quality improvement coaches and has been adopted by two further NEL practices. The same provider also improved triaging by the introduction of a Duty Doctor “Hot Triage” model, with a GP based in reception who clinically triaged all appointment requests and urgent queries.
Click here to learn about the accessible market-leading websites that My Surgery Website can create for you.
-
Providing Information: one practice had a focus on building trust to improve childhood vaccine rates through clinician-led workshops, community discussions and one-to-one nursing support. Feedback highlighted concerns about autism, allergies, neurological conditions and online misinformation. There was a dedicated healthcare assistant contacting hesitant families, and targeted recalls in community languages.
- Listening to and involving people: Another practice had a “You Said, We Did” poster so patients could see the impact of their feedback.
Well-led:
-
Partnerships and communities: One practice reflected on the ongoing impact of Covid lockdowns by creating a community garden with patient help. Collaboration with the local wildlife trust saw it do 5 funded walks per year. One service had developed a brand new enhanced frailty service with a GP partner.
-
Learning, improvement and innovation: Interestingly, Artificial Intelligence appears more than usual this month. One outstanding practice had implemented AI which had increased efficiency, saved time and correlated with increased patient satisfaction scores.
Click the image below to download the full report
SOME 'REQUIRES IMPROVEMENT' / 'INADEQUATE' RATINGS:
Safe:
-
Safeguarding: safeguarding policies were in place but the policies made no reference to human trafficking or radicalisation.
- Safe environments: a business continuity plan was in place but it did not include telephone contacts for essential services such as electricity, gas and water.
-
Medicines Optimisation: this remained a huge area for poor and very poor comments, including where a service did not have a policy in place relating to SGLT‑2 medications.
Our market leading compliance software FPM Core lets you know who has read what policies, and when, so you are always up to date with compliance - click here to book your demo today
Well-led:
-
Capable, compassionate and inclusive leaders: Staff were only made aware of changes to the sickness policy after it had been implemented. This was disclosed to staff via an email informing them of a new policy on Team Net. Staff told us communication from management was ineffective. They had suggested other forms of communication to management; however, they did not feel this was working well. Leaders told us they felt staff remained unhappy with communication and they were not sure how this could be resolved. At another practice, leaders were not following their own policies, specifically in relation to recruitment and grievances.
-
Freedom to speak up: We saw that at the time of our assessment staff had engaged with the freedom to speak up guardian. Following our site visit we were informed the practice had removed this person from the role. We asked for a process and rationale around this decision, given leaders knew that staff had spoken up. Practice leaders were unable to demonstrate they had considered the impact this would have on staff. We were made aware by an external stakeholder that they had suggested a different person for the role of freedom to speak up guardian. The practice then changed the name of the guardian on their policy before informing this person. At the time of writing the practice does not have a freedom to speak up guardian in place.



Jonathan Thank you these short examples are very helpful. KR Steve